The Opportunity
In today’s healthcare climate, unpaid family caregivers are increasingly being expected to provide complex care for their loved ones with little to no training and often while working full-time. These tasks include coordination of health care and social services, medication management and administration, personal care and hygiene, wound care, managing disease-related symptoms, and monitoring medical equipment such as feeding tubes and intravenous infusions. Women are disproportionally affected as much of the burden of family caregiving falls to them for both their children and older loved ones. Caregivers often turn when feeling overburdened or fatigued. Unfortunately, today’s health system is ill-prepared to address the educational, emotional and supportive needs of caregivers and their care recipients. According to a 2015 survey conducted by the National Alliance for Caregiving and AARP, only 1/3 of caregivers reported that a health care provider asked them about their needs when caring for their loved one, and even fewer reported (16%) a health care provider had conversations about caregiver self-care. With many family caregivers facing the challenges of their own aging, it is imperative to identify and advance more comprehensive, cross-disciplinary caregiver support solutions—that address the needs of both caregivers and recipients of care.
Our Goal
In an effort to address gaps in support for family caregivers, we are collaborating with the Center to Advance Palliative Care (Icahn School of Medicine at Mount Sinai) to develop training modules and an operational toolkit for health care providers that identify, address and support family caregivers of individuals with dementia.
Caregivers News
 January 28, 2019
January 28, 2019
d.health Summit 2019
 March 26, 2018
March 26, 2018
New Survey Finds Large Number of People Skipping Necessary Medical Care Because of Cost
 January 11, 2018
January 11, 2018
Health Affairs: A Study Of Family Caregiver Burden And The Imperative Of Practice Change To Address Family Caregivers’ Unmet Needs
 May 23, 2017
May 23, 2017
HuffPost: How to Navigate Successful Aging
Publications and Resources
Our Current Projects
Research
Research
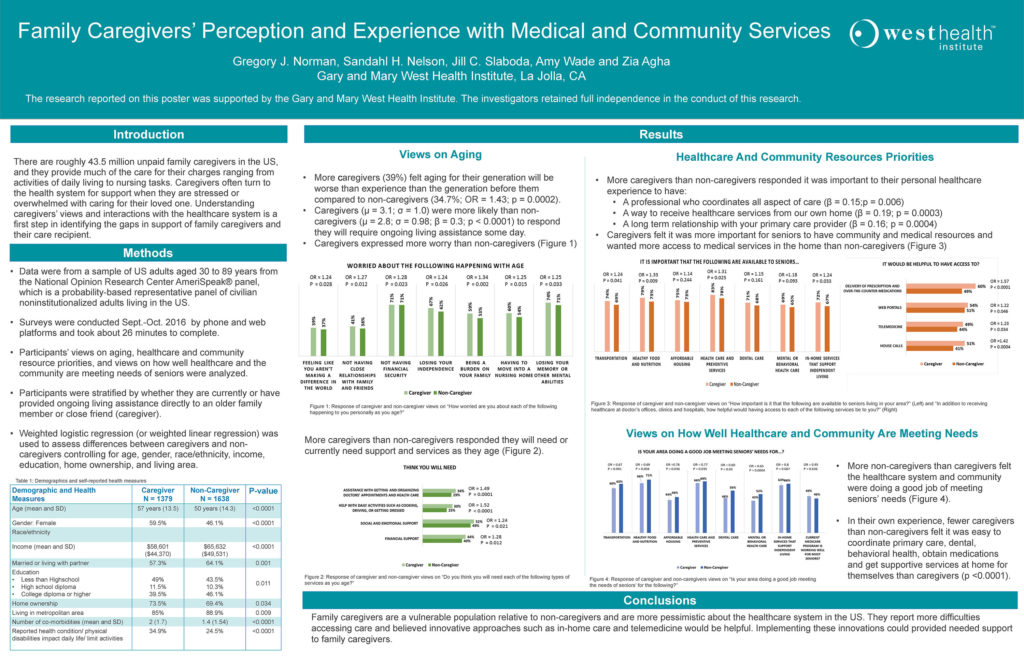
The Institute partnered with NORC to develop and administer a survey to over 3,000 US adults, which asked participants about their opinions, perspectives, and experiences with the American healthcare system. Nearly half (46%) the sample reported currently or previously have been a caregiver to an older family member or close friend. Caregivers were more likely to value health care services that were delivered in the home such as home-based primary care, telehealth medicine, and pharmacy home delivery compared to non-caregivers. Similarly, caregivers valued a long-term relationship with their primary care provider more than non-caregivers. As the health system begins to test and implement innovative care models, the perspective of caregivers should be included since, as we saw in this national sample, caregivers are often dealing with their own multiple chronic conditions while caring for an older adult with significant functional limitations and health problems.
Collaboration
Collaboration
The Institute and the Center to Advance Palliative Care (CAPC) are working with national leaders in dementia care to develop training for all providers who encounter individuals with cognitive impairment and their caregivers. Training will include online clinical courses in the skills needed to disclose a dementia diagnosis to patients, assessing and alleviating caregiver burden, communicating about what to expect as dementia progresses, and interpreting and addressing behavioral symptoms of dementia.